All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit Know GvHD.
The GvHD Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the GvHD Hub cannot guarantee the accuracy of translated content. The GvHD Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The GvHD Hub is an independent medical education platform, sponsored by Medac and supported through grants from Sanofi and Therakos. Funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View GvHD content recommended for you
NIH Consensus Task Force on atypical chronic GvHD following allo-HSCT: New diagnostic criteria and future research prospects
Do you know... Which one of the following is proposed as a diagnostic criterion for atypical cGvHD according to a recent NIH Consensus Task Force report?
Managing atypical manifestations of chronic graft-versus-host disease (cGvHD) in patients who have undergone transplant can be challenging in the context of rare and heterogeneous signs and symptoms.1 Between 2005 and 2020, the United States National Institutes of Health (NIH) held a series of consensus projects considering GvHD. In 2020, as part of the NIH cGvHD Consensus Project, one of the working groups (Working Group IV) focused on atypical features of the disease, considering forms with higher-than-normal morbidity and those that affect unusual systems, such as the skin and eyes.1 Published in Transplantation and Cellular Therapy in May 2022 by Cuvelier at al.1, here we review the formal report from the task force.
Introduction
cGvHD is a leading cause of late morbidity and non-relapse mortality following allogeneic hematopoietic stem cell transplant (ASCT). Treatment of cGvHD is often ineffective, with incomplete responses and recurrence as common outcomes. In the context of atypical cGvHD, late recognition, paucity of experience in management, and a lack of research mean these features can lead to significant morbidity and frequent treatment failure.
The aims of the NIH cGvHD Consensus Project were as follows:
- To generate a summary of current knowledge and understanding of atypical cGvHD features.
- To produce provisional diagnostic criteria for manifestations suspected to be related to cGvHD.
- To identify gaps in current knowledge around atypic cGvHD.
- To propose research ideas and identify unmet needs to guide future research.
Pathophysiology of atypical cGvHD
cGvHD is caused by the systemic failure of immune tolerance to an allogeneic hematopoietic chimera, with immune dysregulation and intolerance of the host by the novel donor immune system. This manifests in cGvHD as both antirecipient alloreactivity and autoreactivity. The study report considers evidence that supports the presence of both processes in cGvHD, including the evidence below:
- The evolution of oligoclonal T cells to recognize both donor and host antigens.
- The presence of established triggers of autoimmunity, including epitopes and molecular mimicry.
- Loss of B-cell tolerance is commonly observed.
- The efficacy of drugs targeting immune tolerance (e.g., corticosteroids) in treating cGvHD.
- The presence of both donor and recipient chimera in plasma.
- The challenges in identifying whether GvHD is caused by alloreactivity or autoreactivity, including diagnostic challenges in identifying effector mechanisms and target cells.
Signs and symptoms of atypical cGvHD
A major challenge for clinicians is recognizing and therefore diagnosing atypical cGvHD; often a sign or symptom is attributed to an etiology not related to cGvHD. The task force identified that this is especially difficult when atypical features occur in the absence of established cGvHD signs, such as nephritis. The report declares that in this context, atypical features should be described as “possibly” related to cGvHD. This is distinct from referring to atypical features as “definitively” related to cGvHD when they manifest in the presence of a confirmed diagnosis according to established cGvHD criteria (Figure 1).
Figure 1. Typical and atypical manifestations of cGvHD*
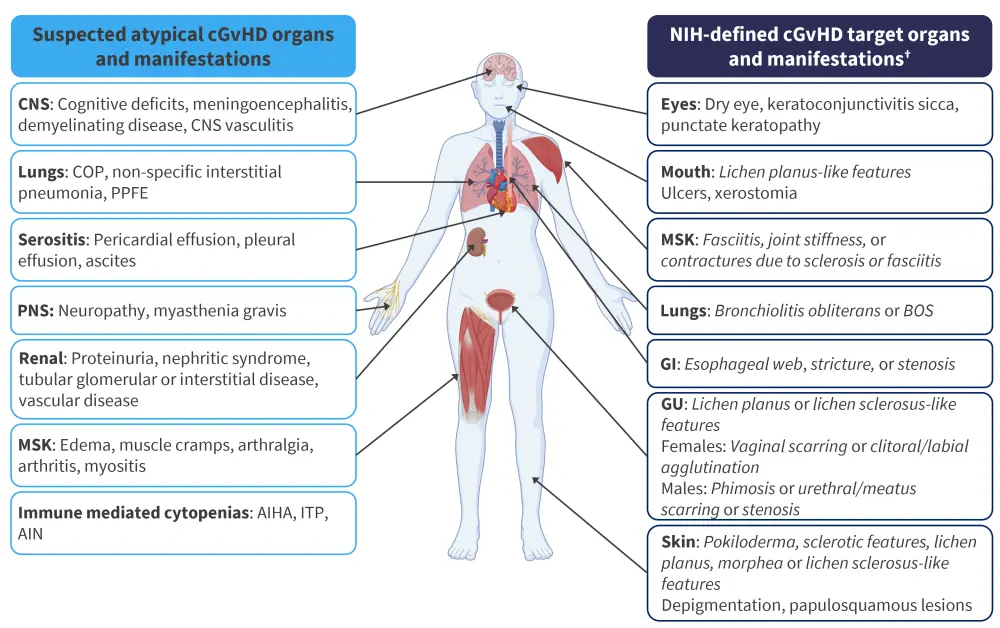
AIHA, autoimmune hemolytic anemia; AIN, autoimmune neutropenia; BOS, bronchiolitis obliterans syndrome; cGvHD, chronic graft-versus-host disease; CNS, central nervous system; COP, cryptogenic organizing pneumonia; GI, gastrointestinal; GU, genitourinary; ITP, immune thrombocytopenia purpura; MSK, musculoskeletal system; NIH, National Institutes of Health; PNS, peripheral nervous system; PPFE, pleuroparenchymal pulmonary fibroelastosis.
*Adapted from Cuvelier, et al.1 Created with BioRender.com.
†For the NIH-defined target organs and manifestations, diagnostic features are in italics and distinctive features are in roman text.
Provisional diagnostic criteria for atypical manifestations of cGvHD
A main aim of the task force was to propose provisional diagnostic criteria for atypical GvHD manifestations, which are presented in Figure 2. Though manifestations can occur throughout the body, neurological, renal, pulmonary, musculoskeletal, and hematologic effects predominate.
Figure 2. Proposed diagnostic criteria for atypical manifestations of cGvHD*
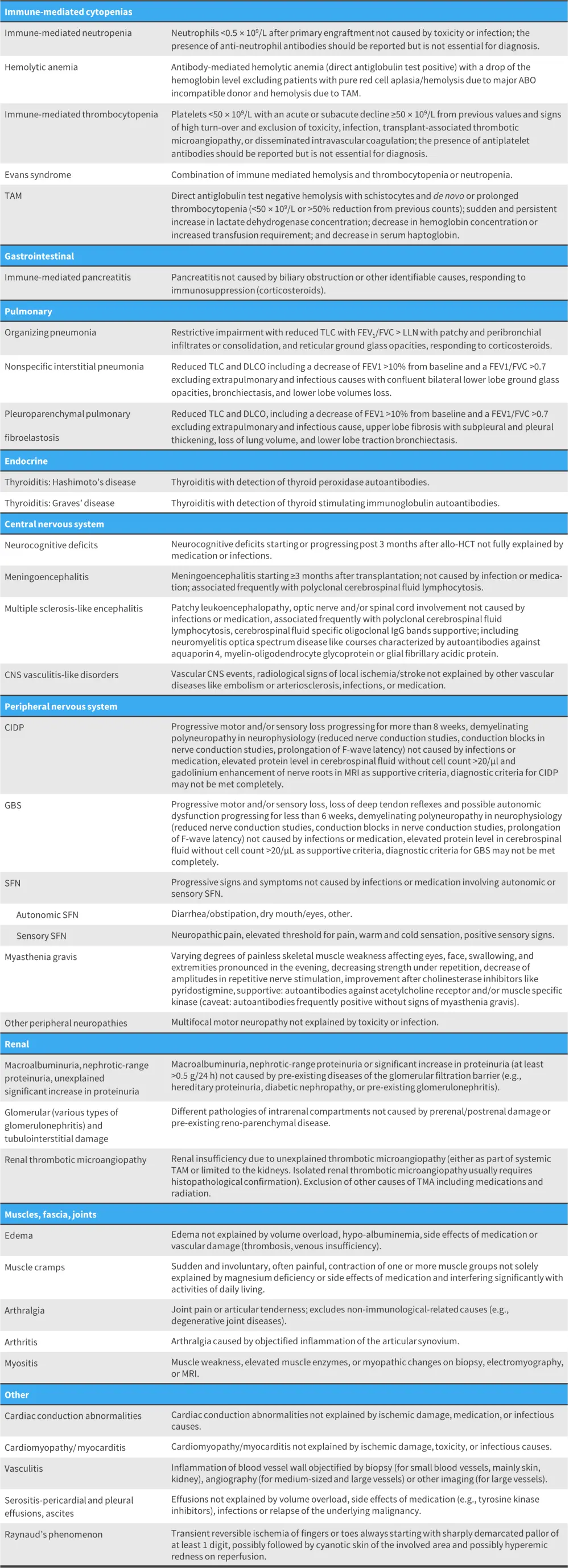
Allo-HCT, allogeneic hematopoietic stem cell transplant; CIDP, chronic inflammatory demyelinating polyneuropathy; CNS, central nervous system; DLCO, diffusing capacity for carbon monoxide; FEV-1, forced expiratory volume in 1 second; FVC, forced vital capacity; GBS, Guillain Barré syndrome; MRI, magnetic resonance imaging; SFN, small fiber polyneuropathy; TAM, transplant-associated microangiopathy; TLC, total lung capacity; TMA, thrombotic microangiopathy.
*Adapted from Cuvelier, et al.1
Potential diagnostic investigations for atypical cGvHD
The review also considers current diagnostic challenges and which sequence investigations can be used to guide diagnosis of atypical cGvHD (Figure 3).
Figure 3. Investigations for atypical cGvHD*
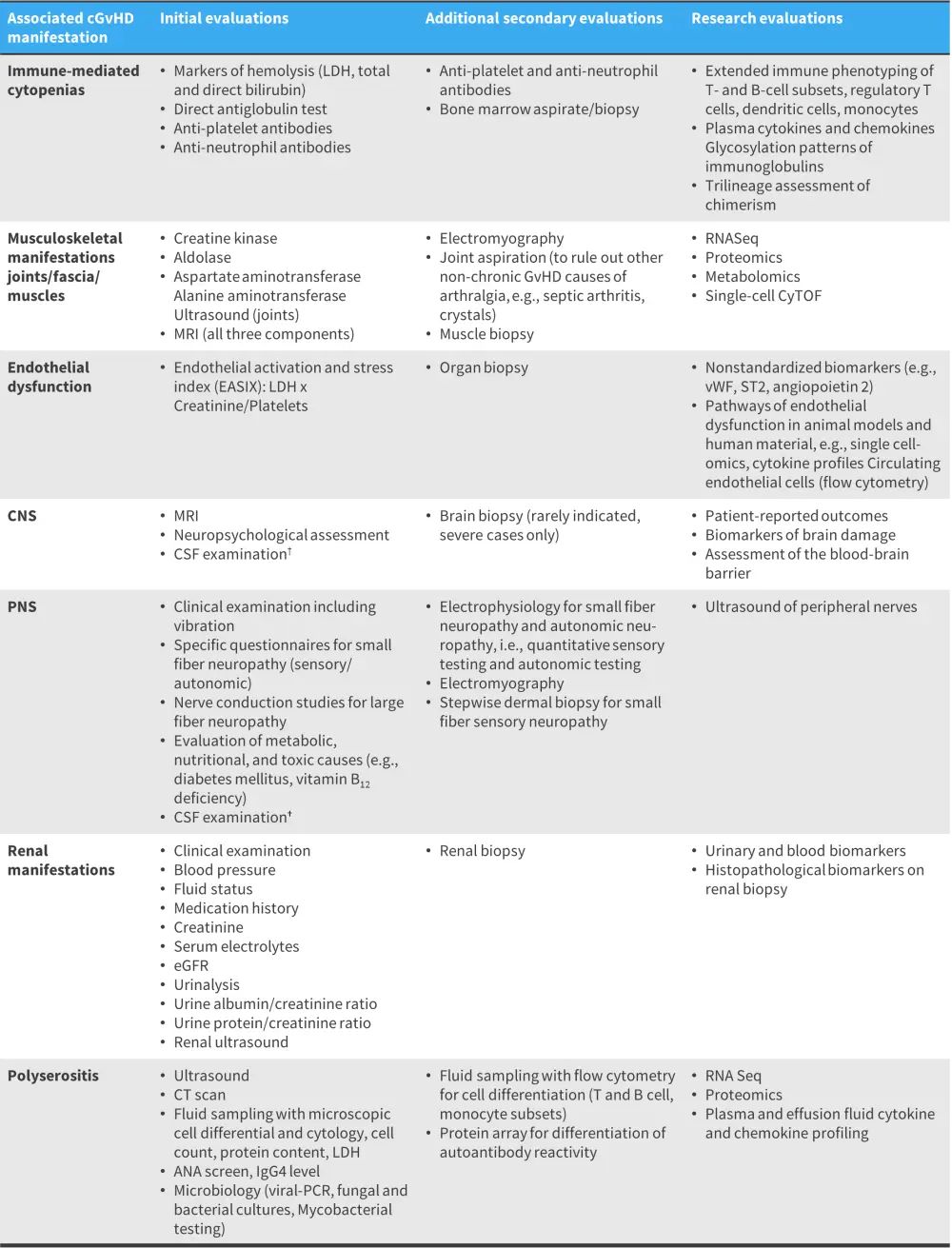
ANA, anti-nuclear antibody; cGvHD, chronic graft-versus-host disease; CNS, central nervous system; CSF, cerebrospinal fluid; CT, computed tomography; CyTOF, cytometry by time of flight; eGFR, estimated glomerular filtration rate; LDH, lactate dehydrogenase; PCR, polymerase chain reaction; PNS, peripheral nervous system; RNA Seq, RNA sequencing; vWF, von Willebrand factor.
*Adapted from Cuvelier, et al.1
†CSF examination: CSF cell count including white blood cell count and differential; CSF lactate, CSF protein; CSF and blood correlation of albumin, IgG, IgA, and IgM; isoelectric focusing; myelin basic protein; and appropriate CSF microbiological and studies (e.g., human herpes virus-6).
Current knowledge and further research for atypical cGvHD
Finally, the review discusses where further research is needed given the atypical features that have been described.
Immune-mediated cytopenia
Immune-mediated cytopenias (IMCs) are well-recognized sequalae in patients who have received ASCT, with a lack of clearly defined incidence to diagnostic uncertainty and lack of systematic reporting. It is also established that osteoblast injury in either acute GvHD or cGvHD can contribute to decreased hematopoiesis. Numerous immune-mediated mechanisms exist to suggest GvHD drives IMC, including ABO incompatibility, loss of immune tolerance, circulating soluble B cell-activating factors, and ineffective T-cell regulation, with a strong association with HLA-mismatched and unrelated donors.
IMCs can occur in the context of donor–donor reactivity or recipient–donor reactivity, suggesting that either immune-mediated mechanisms or cGvHD can lead to the same result. On this basis, the authors advocate that IMC should not be described as autoimmune or alloimmune, but as a “cGvHD-associated immune-mediated cytopenia.”
Further research ideas
- Investigating which biological mechanisms contribute to immune intolerance towards hematopoietic cells.
- Assessing how regulatory T cells and B cells influence peripheral immune tolerance.
- Identifying how mixed donor–recipient chimerism and the type/intensity of conditioning regimen may drive IMCs.
- Evaluating whether blood biomarkers (e.g., skewed Th2/Th1 cytokine profiles) are able to predict a patient’s risk of developing an IMC following ASCT.
Musculoskeletal problems
Atypical cGvHD symptoms include joint pain, muscle cramps, edema, and restricted joint movement (Figure 2). These can be difficult to distinguish from treatment-related problems, such as steroid- or radiation-induced avascular necrosis or steroid-related myopathy, with heterogeneity and rare forms (e.g., myocarditis) complicating the investigation and diagnosis further. Comprehensive investigation, including blood test, autoimmune screening, radiological investigation, physical examination, clinical history, and muscle biopsy, are required. cGvHD-associated myositis, presenting as peripheral nervous system disease in often heavily pretreated patients, can be particularly challenging, with muscle biopsy described by the consensus review as the “standard of care.”
Further research ideas
- Prospective research into the non-invasive assessment of muscles, fascia, joints, and periarticular areas, including evaluation of fibrotic versus inflammatory changes (e.g., different imaging modalities).
- Research into the impact of musculoskeletal cGvHD on linear growth in prepubertal children, including comparison with rheumatological conditions.
- Biobanking of rare and valuable tissue samples (e.g., muscle biopsies).
- Advanced/deep genomic studies of biological samples (e.g., bulk RNA sequencing, novel unbiased epigenomic, transcriptomic, proteomic and metabolomic assays).
Endothelial damage
The atypical endothelial manifestations of cGvHD include avascular areas of skin, neovascularization, and enlarged capillaries. Similar to established GvHD complications, such as thrombotic microangiopathy, these endothelial changes arise from an interplay between proinflammatory cytokines, upregulation of endothelial cell adhesion molecules, migration of lymphocytes, and activation of platelets and coagulation factors. In addition, steroids and other traditional treatments used for cGvHD may cause further endothelium damage. Both coronary and peripheral artery disease related to endothelial injury have been clearly identified in patients with cGvHD, as has organ and tissue injury, including of the skin.
Further research ideas
- The development of animal models to delineate the pathophysiology of endothelial dysfunction that occurs in cGvHD.
- The use of animal models to develop interventions for endothelial protection, angiogenesis, and neovascularization.
- The validation of clinical biomarkers of endothelial dysfunction in patient cohorts.
- To determine the utility of non-invasive imaging in endothelial dysfunction, including flow-mediated dilation, reactive hyperemia, or digital photoplethysmography.
Central nervous system and peripheral nervous system
Evaluation of the effects of cGvHD on the central nervous system (CNS) is complicated by pre- and comorbid conditions, as well as medications that affect the CNS and cognitive function. Rare complications, such as cGvHD-associated acute disseminated encephalomyelitis (ADEM), have been described, but the prevalence of true cGvHD-associated CNS impairment remains to be elucidated. While neurocognitive impairment has been clearly described in patients undergoing ASCT, the role of cGvHD is unknown. Putative processes have been described, including cytokine overproduction, T‑cell infiltration, granulomatous changes, and antibody-mediated encephalopathy.
The peripheral nervous system (PNS) manifestations of atypical cGvHD that have been described include immune-mediated Guillain-Barré syndrome, myasthenia gravis, and chronic inflammatory demyelinating polyneuropathy, among others (Figure 2). As with the musculoskeletal manifestations of atypical cGvHD, these can be difficult to distinguish from treatment complications, including drug-related neuropathy, paraneoplastic, and infection-related complications. The PNS symptoms described by patients include positive sensory symptoms (e.g., pain or paresthesia) or negative sensory symptoms (e.g., numbness). They can also include physical symptoms, with autonomic manifestations such as sweating and muscle cramps. A range of investigations exist with the aim of determining the underlying cause of peripheral neuropathy in patients.
Further research ideas
- Comprehensive, prospective, observational studies that include neuroimaging, neuropsychological assessment, and patient-reported outcomes to the assess longitudinal central CNS changes with GvHD.
- The development of biomarkers relating to the integrity of the blood–brain barrier to assess response to treatment (e.g., neurofilament light chain).
- The development of experimental models to distinguish toxic- from immune-mediated neurological damage.
- The development of standardized diagnostic criteria and non-invasive diagnostic tools specific to cGvHD peripheral neuropathy.
- The development and validation of patient-reported outcome measures that can guide longitudinal observational studies and routine care of patients with cGvHD, including identifying patients requiring neurologic testing for autonomic neuropathy and autonomic disturbances, small fiber neuropathy, and muscle cramps.
- The investigation of biomarkers that indicate immunologically-mediated peripheral nerve damage to clarify the pathophysiology.
Renal manifestations
Evaluation for possible renal cGvHD requires comparison of current renal function against renal function both before and early after ASCT. Evaluation before transplantation should include consideration of nephrotoxic exposures, such as medications (e.g., aminoglycosides) and pre-existing renal conditions
Further research ideas
- The implementation and validation of guidelines for monitoring renal function in patients after transplantation.
- The development of large, prospective, multicenter studies to capture the incidence of renal injury with cGvHD, and to facilitate central biobanking of valuable renal biopsy, blood, and urines samples, in particular to aid omics studies and the development and validation of biomarkers.
- The development of clear clinical and pathology consensus definitions and classification systems for renal cGvHD.
Polyserositis
Polyserositis is rare, manifesting as localized effusions, including pleural and pericardial effusions and ascites. It is a diagnosis of exclusion as it shares this clinical presentation with other transplant-related complications, such as microangiopathic anemia. The pathophysiology of the condition remains poorly understood but it is associated with increased levels of different white cells in effusion fluid and peripheral blood.
Further research ideas
- The establishment of large, multi-institution projects to collaborate on the generation of clinical data, biobank samples (e.g., mononuclear cells and plasma from peripheral blood and effusions), and registry data.
Conclusion
The report from the 2020 NIH Consensus Project Task Force clearly proposes provisional diagnostic criteria for the assessment and diagnosis of atypical cGvHD in patients who have undergone transplant. Though rare and heterogenous, these manifestations can carry considerable morbidity risks for patients and treatment challenges for clinicians.
To better manage these patients, large, multicenter, prospective studies, including biobanking and the development of clinical and pathological criteria, are required to improve understanding of the underlying pathological processes.
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content

